Infertility Treatment
- Over 20 Years Of Experience- Locally Owned- Free Consultations
Chicago Infertility Associates provides infertility treatment to the greater Chicagoland, IL area. Our experts are compassionate about your infertility issue and you can count on our specialized treatments. We are a part of the American Medical Association and the BBB and our goal is to provide you with the best fertility and gynecological care.
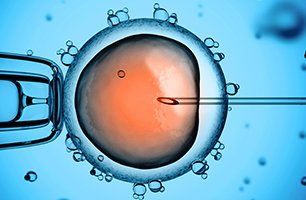
IVF
At Chicago Infertility Associates we offer thorough and specialized IVF services. Our services are designed to provide reliable fertility and gynecological care. Call
us for a FREE consultation.
Learn More
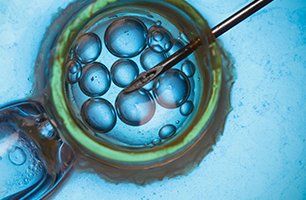
ICSI
Our experts are well informed about various fertilization issues and understand patient problems individually. Our treatments are research-based and reliable.
Learn More
PGD
We offer all PGD services and utilize pre-implantation genetic diagnostic technology for analyzing genetic make-up of the early embryo before transferring it into the uterus.
Learn More
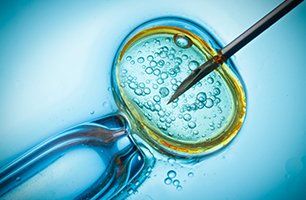
Assisted Hatching
This technique involves measuring the thickness of the zona pellucida in embryos that are candidates for the procedures. Call
us for a FREE consultation.
Learn More
Surrogacy
We offer various egg donation and surrogacy programs at Chicago Infertility Associates, along with this you can also undertake the donor egg program eligibility questionnaire.
Learn More
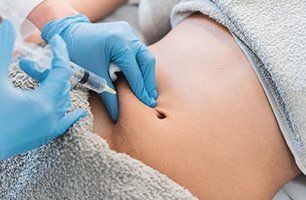
Gonadotropins
Fertinex, Follistim, Gonal-F, Pergonal, and Repronex – These compounds are human hormones produced by the pituitary gland (LH and FSH) and are used to stimulate ovarian follicular development. Visit
us today.
Learn More



Share On: